Clinical documentation consumes more physician time than any other administrative task. Research shows doctors spend two hours on electronic health record tasks for every hour of direct patient care. That ratio inverts the fundamental purpose of medical practice.
The workload follows physicians home. Evening charting sessions replace family dinners. Weekend documentation catches up steal personal time. Vacation days include logging into the EHR from hotel rooms. This pattern drives burnout rates to record highs across all specialties, , according to the latest physician burnout statistics.
AI medical charting technology eliminates this burden. An AI SOAP note generator listens to patient conversations and creates complete clinical documentation automatically. No typing required. No evening catch up sessions. No memory gaps from delayed charting.
Physicians who implement this technology reclaim 10 hours weekly. That represents an entire workday returned to clinical care, family time, or personal recovery. Here’s exactly how the system works and how to start using it immediately.
What is an AI SOAP Note Generator?
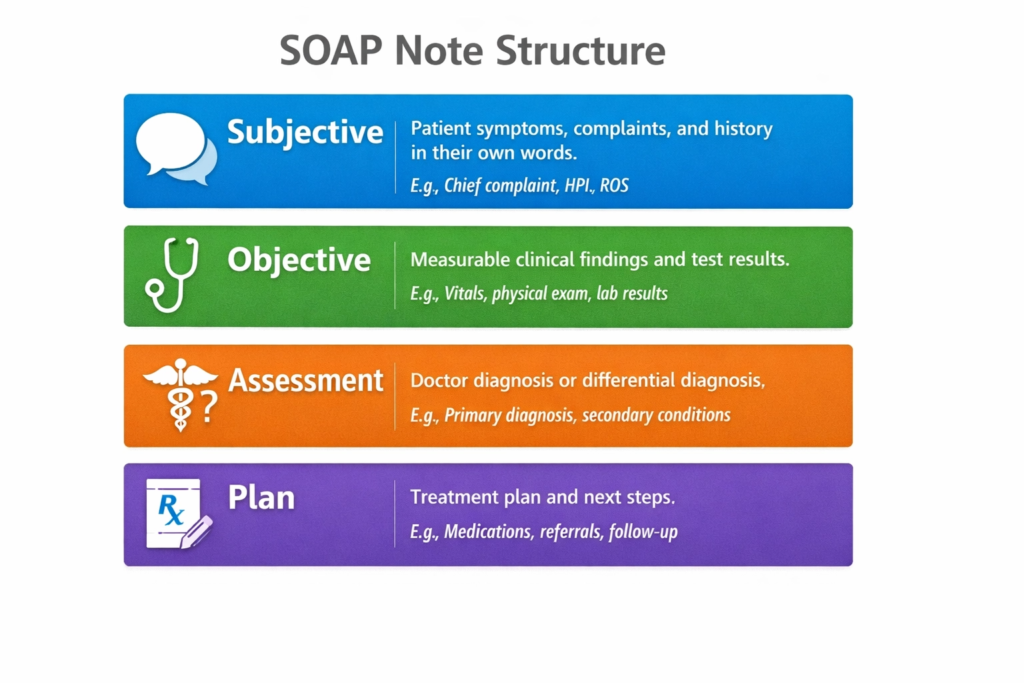
An AI SOAP note generator is software that listens to doctor patient conversations and writes medical notes automatically. The system captures everything discussed during the appointment and organizes it into the standard SOAP format without any typing.
Think of it as having an invisible medical scribe in every exam room. The software sits quietly in the background during appointments. It understands medical terminology. It knows which information belongs in each section of the chart. It generates complete documentation the moment the visit ends.
The technology operates under strict HIPAA compliance with Business Associate Agreements and encryption protecting all patient data. No audio recordings get stored permanently. No patient information trains public AI models. Everything disappears after the note reaches your EHR system.
Understanding how virtual medical scribes work provides useful context for how AI documentation differs from traditional human scribes.
How Does an AI SOAP Note Generator Work?
Modern automated SOAP notes work nothing like old dictation software. You never say “comma” or “period” or “new paragraph” out loud. You speak naturally with patients exactly as you normally would. The AI handles everything else.
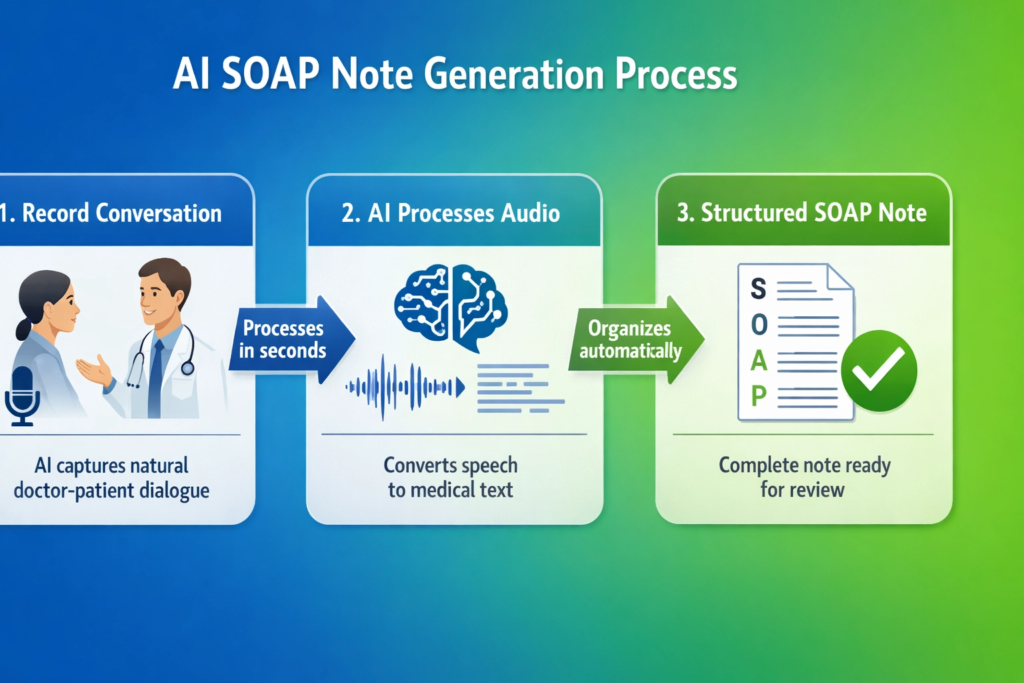
The process breaks down into three distinct steps that happen seamlessly in the background.
Step 1: Recording the Conversation
Documentation starts when the AI app opens on your phone, tablet, or computer. Simply press record and the software begins capturing audio immediately. The device can sit on a counter or stay in your pocket. Modern systems work from several feet away without special microphones.
The conversation proceeds normally. Ask about symptoms while the patient describes their concerns. Discuss treatment options as family members ask questions. Throughout all of this, the software captures everything without interrupting the natural flow of communication.
Maintaining eye contact with patients throughout the entire visit becomes easy. No laptop screen creates a barrier. No typing breaks the connection. The appointment feels like actual medicine instead of data entry with occasional patient interaction.
Step 2: Converting Speech to Medical Text
The AI processes your recording using language models trained specifically on millions of medical conversations. These models understand healthcare vocabulary that confuses general speech recognition software.
The system performs speaker separation, meaning it can tell your voice apart from the patient’s voice and any family members in the room. This matters because the AI needs to know who said what to organize information correctly.
Medical terminology gets transcribed accurately. Drug names like lisinopril or atorvastatin. Diagnoses like erythematous mucosa or anterior cruciate ligament tear. Procedures like cholecystectomy or arthroscopy. The AI recognizes thousands of medical terms without confusion.
The software also filters out irrelevant conversation. Small talk about weather or traffic doesn’t appear in the final note. Only clinically relevant information makes it into documentation.
Comparing medical dictation vs medical scribe options helps clarify why AI transcription offers advantages over traditional dictation software.
Step 3: Organizing Information into SOAP Format
Raw transcription produces pages of unstructured text. Nobody wants to read a three page conversation transcript to find key clinical details. The AI solves this by automatically organizing information into proper SOAP structure.
Subjective sections capture the patient’s complaint and symptoms in their own words. History of present illness gets summarized clearly. Review of systems includes only relevant positives and negatives discussed during the visit.
Objective sections record vital signs, physical exam findings, and any test results mentioned. Based on medical documentation standards, the AI knows these belong in Objective rather than Subjective.
Assessment sections state your diagnosis or differential diagnosis based on the clinical evidence discussed. From the conversation flow, the AI can infer your diagnostic reasoning.
Finally, Plan sections itemize next steps including prescriptions, referrals, lab orders, imaging studies, and follow up instructions. Everything you told the patient about their treatment gets captured in clear action items.
The complete note appears within seconds of ending the recording. You review it briefly for accuracy, make any needed adjustments, and approve it. The entire process takes 60 seconds instead of 5 to 15 minutes of typing.
Top 5 Benefits of Using AI for Clinical Notes
Automated documentation changes more than just how notes get written. It transforms the entire practice experience for both physicians and patients.
Benefit 1: Get 10 Hours Back Every Week
Manual charting takes 5 to 15 minutes per patient depending on complexity. Multiply that across 25 to 40 patients daily and you lose hours every single day to documentation. Research on EHR documentation burden confirms physicians allocate nearly two hours to administrative work for every hour of patient care. Most of that time happens after clinic hours because completing charts between patients disrupts workflow.
AI reduces charting time to 60 seconds of review and approval per patient. The time savings compound quickly. Five minutes saved per patient across 30 patients daily equals 150 minutes, which is 2.5 hours. Over a five day week, that becomes 12.5 hours reclaimed.
Those hours return to your life immediately. You leave clinic on time. Evenings belong to family instead of the EHR. Weekends happen without documentation backlog hanging over you.
Benefit 2: Actually See Your Patients During Visits
Traditional documentation forces physicians to choose between eye contact and thorough charting. You either type during the visit and ignore the patient, or you skip documentation and do it later from memory.
Neither option serves anyone well. Patients feel dismissed when you stare at a screen. Clinical details get forgotten when charting happens hours after the encounter. The provider patient relationship suffers while documentation quality declines.
AI removes this impossible choice. Maintaining full attention on the patient throughout the appointment becomes natural. Reading body language happens effortlessly. Catching subtle expressions that signal anxiety or confusion improves care quality. Building therapeutic rapport that improves outcomes becomes the focus.
The patient experiences what medicine should feel like. A doctor who listens completely. A conversation without constant interruption for typing. Care that feels personal rather than transactional.
Benefit 3: Eliminate Burnout from Documentation
Documentation burden ranks as the leading cause of physician burnout according to every major study on the topic. The endless charting creates a sense of never being finished. Work follows you home every night. Time off still includes EHR login sessions.

Such patterns destroy physician mental health and drive early retirement. Experienced clinicians leave medicine entirely because administrative work makes clinical practice unsustainable.
AI breaks the cycle immediately. Charts finish when patients leave. Nothing carries over to evening or weekend. For once, vacation actually means vacation without laptop requirements.
Physicians report dramatic improvements in job satisfaction within weeks of implementing automated documentation. The weight of constant charting simply disappears.
Reviewing the pros and cons of medical scribes shows how AI documentation compares to hiring human scribes for your practice.
Benefit 4: Capture More Revenue Through Better Documentation
Physicians often under code visits because manual documentation makes thorough charting too time consuming. You skip minor details that justify higher level billing codes. Small elements of the history or exam don’t make it into notes.
This undercoding costs thousands of dollars monthly in lost revenue. You perform E&M level 4 work but bill level 3 because your documentation doesn’t reflect everything you actually did.
AI captures every detail discussed during the visit. Nothing gets forgotten or skipped for time reasons. The documentation finally matches the actual clinical work performed.
Many practices see immediate increases in appropriate billing levels after implementing AI documentation. The software pays for itself through improved revenue capture alone.
Benefit 5: Document Accurately While Memory is Fresh
Charting from memory hours or days after the visit guarantees clinical details get lost. You forget which medication the patient already tried. You miss important family history mentioned in passing. You confuse details between similar patients seen on the same day.
These memory gaps create documentation errors that affect future care decisions. They also expose practices to liability when charts don’t reflect what actually happened during visits.
AI generates notes the moment encounters end. Every detail gets captured with perfect accuracy. No memory degradation occurs. Charts precisely reflect conversations that just happened.
This immediacy improves both clinical quality and legal protection. Future providers reading the chart get complete information. Malpractice defense becomes easier when documentation proves exactly what transpired.
Integrating an AI SOAP Note Tool with Your Existing EHR
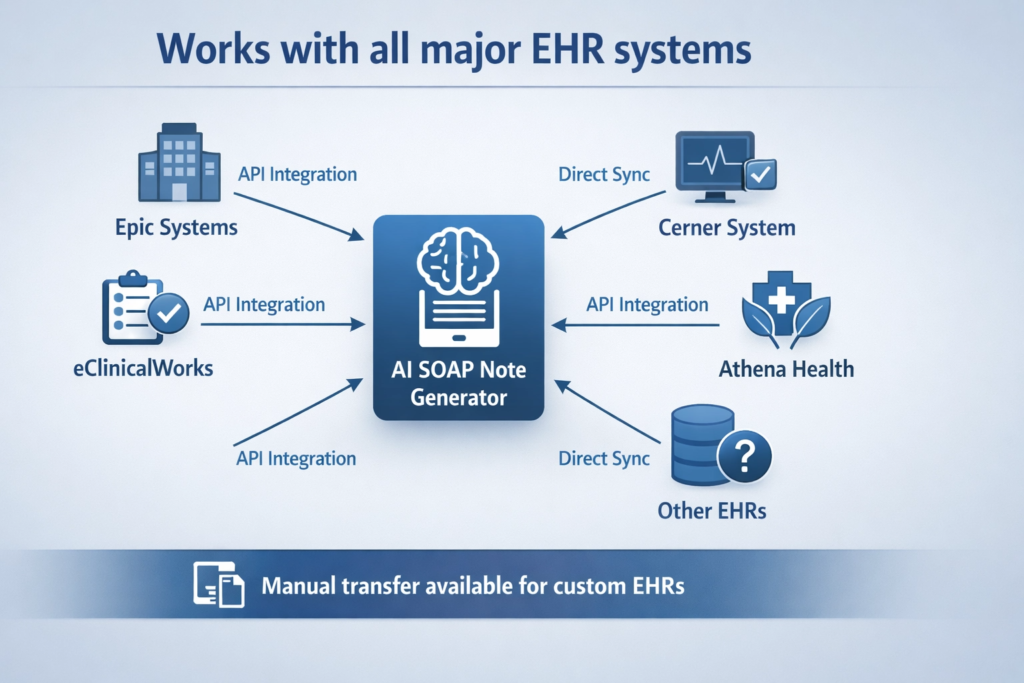
The most common implementation concern is EHR compatibility. Practices worry the AI won’t work with their specific electronic health record system.
Most modern AI SOAP note generators integrate directly with major EHR platforms including Epic, Cerner, Athenahealth, eClinicalWorks, and dozens of others. Direct integration means the AI pushes completed notes into your chart with a single click.
The technical connection happens through API integration. Your IT department or the AI vendor handles the setup process. Once configured, the workflow becomes seamless. You generate the note in the AI system, review it, approve it, and it appears in the patient’s chart immediately.
Practices using less common or highly customized EHR systems still have options. Nearly all AI tools support copy and paste transfer. You generate the note in a separate window, review it for accuracy, copy the text, and paste it into the appropriate fields in your EHR.
Because AI notes arrive perfectly formatted and organized, even copy and paste takes only seconds instead of minutes. The note drops directly into place without reformatting or reorganization.
Security and compliance concerns get addressed through Business Associate Agreements that make the AI vendor legally responsible for HIPAA compliance. Data encryption protects information during transmission and storage. Zero retention policies guarantee patient data never remains on vendor servers after notes transfer to your system.
Understanding medical scribe duties and scope of practice clarifies what AI systems can and cannot do compared to human medical scribes.
Why ScribeRunner is the Best AI SOAP Note Generator for 2026
The AI documentation market includes dozens of competing platforms. Quality varies dramatically between vendors. Some deliver exceptional results while others produce unreliable output that creates more work than it saves.
After extensive evaluation across multiple specialties and practice types, ScribeRunner consistently demonstrates superior performance for modern healthcare environments.
Clinical Accuracy
ScribeRunner uses healthcare specific language models trained on millions of real medical encounters. The system handles complex medical vocabulary across all specialties without confusion. Rare diagnoses, obscure drug names, and technical procedure terminology all transcribe correctly.
The AI understands context well enough to capture nuance. It recognizes when you discuss past medical history versus current symptoms. It distinguishes between medications the patient takes versus medications you’re prescribing. It tracks multiple conditions discussed during complex visits.
Accuracy rates exceed 98% on medical terminology across specialties. The occasional error that occurs gets caught easily during the 60 second review process.
Speed
Many AI documentation tools take minutes or even hours to return completed notes. This delay defeats the purpose of automation if you still need to complete charts manually and then reconcile them with AI output later.
ScribeRunner delivers structured SOAP notes within seconds of stopping the recording. The note appears while the patient is still in the exam room. You can review and approve it before moving to the next appointment.
This immediate turnaround means charts truly finish when patients leave. No batch processing delays. No waiting for overnight processing. Instant documentation that keeps pace with clinical flow.
Security and Compliance
ScribeRunner operates under strict Business Associate Agreements that transfer HIPAA liability to the vendor. End to end encryption protects all patient data during transmission and storage. Specifically, AES 256 encryption secures data at rest while TLS 1.2 protects data in transit.
Zero data retention policies get enforced platform-wide. Audio recordings and transcripts get permanently deleted immediately after notes transfer to your EHR. Patient information never remains on ScribeRunner servers. Data never trains public AI models.
Role based access controls limit who can view documentation. Multi factor authentication prevents unauthorized access. Automatic session timeouts protect against unlocked devices. Detailed audit logs track every user action for compliance verification.
Ease of Implementation
ScribeRunner integrates directly with major EHR systems through native API connections. Implementation takes days rather than months. Training requirements are minimal because the interface is intuitive.
No special hardware is needed. The software runs on standard smartphones, tablets, and computers. No expensive microphone arrays. No dedicated recording equipment. Just the devices already in your practice.
Support teams provide hands on assistance during implementation and ongoing use. Technical issues get resolved quickly. Questions receive same day responses. Updates roll out automatically without disrupting workflow.
Learning more about the best AI medical scribe software options provides broader context for evaluating different platforms before making a purchase decision.
Frequently Asked Questions
Yes, AI medical scribes like ScribeRunner listen to patient encounters using ambient voice technology and automatically write complete SOAP notes in real time. The software captures natural conversation, extracts clinical information, and organizes it into proper documentation format without any typing required.
No, the standard public version of ChatGPT cannot be used for medical documentation because it violates HIPAA regulations. ChatGPT does not sign Business Associate Agreements, stores conversation data permanently, and uses that data to train its public models. Healthcare providers must use specialized HIPAA compliant AI software designed specifically for medical documentation.
Modern AI SOAP note generators achieve over 98% accuracy on medical terminology and clinical documentation. These systems use language models trained specifically on millions of healthcare conversations, pharmacology databases, and medical literature. Accuracy depends on audio quality, speaker clarity, and complexity of medical vocabulary, but current platforms handle even rare diagnoses and obscure drug names reliably.
Pricing varies by platform and practice size. Individual subscriptions typically range from $99 to $299 per physician monthly. Enterprise pricing for larger practices runs $200 to $400 per physician annually. Most vendors offer free trials allowing practices to test the system before committing. Cost should be evaluated against time savings, the typical physician reclaiming 10 hours weekly generates substantial value that far exceeds software expenses.
No, AI documentation tools assist physicians rather than replace them. The technology handles administrative work so doctors can focus on clinical decision making, patient relationships, and complex medical reasoning that requires human judgment. AI generates draft documentation that physicians review and approve, ensuring clinical accuracy and appropriate medical judgment guide all charting decisions.
Stop Charting at Midnight. Start Living Again.
ScribeRunner’s virtual scribes handle your documentation while you focus on patients.
Why Physicians Choose Us:
✅ 90% complete notes before patients leave
✅ No long term contracts, cancel anytime
✅ Go live in 7 days with your EHR
✅ HIPAA certified with bank level security
Contact ScribeRunner:
- Phone: (786) 866-7849
- Address: 25 SE 2nd Ave, Suite 1030, Miami, FL 33131
- Hours: Monday through Friday, 8 AM to 6 PM EST
- Service Area: Miami, Fort Lauderdale, Tampa, Orlando, and nationwide

